Sleep
Article curated by Ginny Smith
Humans spend roughly a third of our lives doing it, yet scientists still don’t really know what sleep is for, nor why we need it[1]. Yet going without sleep will cause death sooner than going without food, so it must have some incredibly important and evolutionary ancient function...
Some theories suggest that sleep is essential to keep the brain in working order. It may support the organisation of memories, or allow the synapses (nerve junctions) in the brain to be cleared of toxins that build up during the day. Maybe it's just to keep us away from potentially hazardous situations for a length of time... All good reasons, but none of them powerful enough to drive the evolution of sleep, leaving its main function an elusive mystery...

Why do we sleep?
All but the most incredibly basic of animals need to sleep, and yet scientists don't know why this strange state of suspended animation is vital to survival.
Some believe that sleep is a way to conserve energy and stay out of harm’s way[2]. Animals that stay still and quiet during part of the day are less likely to have accidents or be eaten by predators. Sleeping also uses up fewer calories than being awake, meaning animals need to find less food each day than if they don’t sleep[3]. But this only really explains why we rest during the night – surely it would be safer to stay still and quiet but conscious, so that if a predator stumbles upon your hiding place you can escape? Also, this theory might explain why sleep is a good idea, but it doesn't explain all the problems that are caused by missing out on getting enough sleep.
Other researchers think that sleep is when the body repairs itself[4]. This seems plausible – we all feel better after a good night’s sleep. However, this theory seems to suggest that people who are more physically active (and so need more bodily repair) should sleep more than those who are inactive. But although there is some evidence athletes sleep more after a race than normal, those who are completely inactive don’t sleep any less[5].
Most impairments from sleep deprivation are cognitive, suggesting sleep must be important for the brain. There's some evidence that the cells in the brain responsible for repair and restoration are more active during the night[6], so perhaps the brain that needs time to recuperate, not than the body. In mice, a study by scientists at the University of Rochester found that cerebral spinal fluid flows around the brain ten times faster when they're asleep[1]. This flushes out toxins more efficiently. The researchers argue this could explain the need for sleep, and the problems that occur when we don’t get enough of it. But others are sceptical, and there's not yet any evidence in humans[7].
Another theory is that sleep is for storing memories. Researchers are not clear exactly how this happens, or why sleep is needed, but studies have shown that people are better at remembering things after sleep[8]. Yet whilst this explains the cognitive difficulties people face when sleep deprived, it can’t explain the physical symptoms.
Maybe none of these theories are even close, or maybe more than one is needed to fully explain why sleep matters. What we do know, though, is that people who get enough sleep (around 8 hours a night for adults) are healthier, happier and more successful… what better reason to get some shut-eye?
Learn more about Function of Sleep.


 2
2Crucially, however, this isn't true for a small proportion of the population: sleep mutants. Sleep mutants have a gene mutation that lowers natural sleep demand. Several have been discovered: some lower average sleep demand by 20 minutes, whilst others allow the carrier to have a good night's sleep on as little as 4.3 hours. There may be others as yet undiscovered. Scientists are still wondering where these genes came from and how long they've been about: they are rare. Even recently evolved advantageous genes, however, such as the one that lets adults digest milk, spread fast. And these genes are stranegly advantageous: carriers don’t seem to suffer from the myriad of illnesses that otherwise correlate to sleep deprivation, such as obesity or depression. However, we'd need to do longitudinal studies with huge numbers of people to know for sure. Currenty, not enough sleep mutants have been discovered to do this. In the future, scientists might be able to develop drugs that mimic the effects of specific mutations. However, some, such as NPSR1, have other key functions. This gene is involved in stress and fear responses, so mimicking its effects poorly could have devastating effects we can only guess at.


 2
2
How do we sleep?
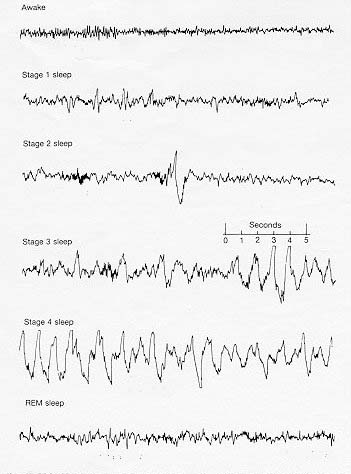
Although we understand how the brain transitions between the stages of sleep that we know about, such as REM, scientists have yet to explain how the brain transitions from wakefulness to sleeping and vice-versa. It is possible that it is a self-organised process where only certain sections of the brain need to be in a sleep-like state to send us to sleep[9], but this is not entirely clear.
As Joshua Fleming so aptly stated on our blog in 2015, for now, the solution to how we sleep is only something we can dream about
.
Learn more about How do we sleep?.

Why do we dream?
Sleep itself may be a mystery, but so are the many strange occurrences that we experience while we sleep – the most well known of which is dreaming. We don't know why we dream, or if it even has an evolutionary benefit, but studies hint at potential reasons.
One idea is that dreams help us process memories which have formed during the day, and convert them into more stable long-term memories[10]. We know that sleep is vital for this process, but whether dreams help isn't clear. Interestingly, young babies spend a higher proportion of their sleep in REM sleep (the phase during which dreams are most likely to occur). As babies learn more rapidly than adults, could this mean they need to dream more to process the information?
Another idea is that dreams help us deal with difficult emotions in a safe way. They may help remove emotions from painful memories so we can recall them without experiencing the emotions as strongly. They may even help prepare us for potential future emotional situations, by letting our brains a rehearse. But this theory is difficult to prove.
One final idea is that dreams aren't 'for' anything at all – they are simply a byproduct of the other vital processes out brain carries out during the night. Will we ever be able to determine which of these theorise is correct, or will dreams remain a mystery? Only time will tell...
Learn more about Why do we dream?.


 4
4
Scientists believe that everyone dreams, but not everyone remembers these dreams when they wake. We don't know exactly why this is, although part of the reason may be that high recallers spend more time awake during the night, suggesting they are more likely to have woken up part way through a dream, which we know increases your chance of remembering it. This isn't enough to explain all the differences, however.
You have the best chance of recalling a dream if asked about it within 5 minutes of waking – after this, much of the detail is lost. So maybe those who remember dreams make an effort to recall them during this window and, in doing so, store them for later. If you want to recall more of your dreams, experts suggest keeping a dream journal, and writing down details in it as soon as you wake. There are also brain differences between low recall and high recall groups. For example, high recallers are more "responsive" to their name being called when awake, and show a greater brainwave change – although the difference doesn't occur when asleep, so it's not clear how it links to dream recall. One brain scanning study found high recallers have more activity in a part of the brain called the temporoparietal junction[11]. The researchers believe this may allow the dreamer to focus more attention on external stimuli, meaning dreams are better embedded in the sleeper's memory.



Some people experience lucid dreaming – dreaming whilst aware that they are dreaming – and some even feel they are controlling the direction of their dreams. It is difficult to know for sure whether lucid dreaming is real sleep, but because it occurs during REM sleep, dreamers can use pre-arranged eye signals to communicate with researchers. We don't know how people are able to control their dreams, nor whether or not this means they're "truly dreaming" or a daydream-like state of semi-wakefulness. The phenomenon warrants further study.

Researchers using fMRI to scan brain activity during dreaming have developed a process that can map the images recalled by the dreamer to a 3-dimensional picture of the brain. Known as “dream decoding”, the process works by repeatedly waking a sleeper and asking what they remember, then pairing this with which bits of the brain light up in the scanner. After over 200 repeats, researchers have been able to use the tool to predict basic objects that appear in the dream[12], including men, words and books. The tool initiaaly was 60-70% accurate, but could be improved with more data.


Strange sleep behaviours
Most of the time when we're asleep, our bodies are inactive. In fact, during REM sleep, our muscles (other than those around our eyes) are actually paralysed. But some people are far from inactive during the night. Sleepwalking is relatively common in children, though we don't know why. It is not usually a symptom of any underlying condition – and most children grow out of it, although some adults do it too. Mostly, it happens during slow wave sleep, when muscles aren't paralysed. It is effectively a state between sleep and wakefulness – a person may walk around with a glazed look or even perform complicated behaviours such as driving. Occasionally, they may become violent and try to hurt themselves or others. When they awake, they usually have no memory of the episode. We don't know what causes sleepwalking, but it's likely to be some kind of disruption to the normal sleep cycle, and is more common when people are sleep deprived. However, when it comes to the old adage that it's dangerous to wake a sleepwalker, scientists disagree about whether it's true!

![Sleepwalker Photograph courtesy Max Pixel [CC0]](/img/sci/sleepwalking-young-red-model-sleep-pillow.jpg)
New research has correlated sleepwalking and other movement during sleep (REM sleep behaviour disorder) with an increased risk of developing dementia with Lewy bodies (proteins in the brain)[13] – the type of dementia seen in Parkinson’s and Alzheimer’s. The correlation is stronger in men than in women, and scientists can’t yet say why.


 2
2In sleepwalking, the body is active but the mind is asleep, but the opposite is also possible, and is known as sleep paralysis. Few have heard of it, but sleep paralysis is actually a common experience, affecting 40% of people at some point in their lives! When we sleep, we go through different phases. In one of these, REM sleep, we experience dreams, our eyes move around rapidly, and the rest of our muscles become paralysed. Sleep paralysis is thought to occur when something goes wrong with this process, and the ‘mind’ wakes up while the body is still asleep and paralysed.
Realising you're paralysed is scary, and scientists believe it's this fear response that causes many people to feel there are other people in the room. It's believed that many reports of ghost sightings, alien abductions and even witchcraft during the historical witch trials may be down to episodes of sleep paralysis! Scientists are still trying to find out why sleep paralysis happens.
Learn more about Sleep Paralysis - A Ghost Story.

Another common sleep phenomenon is the hypnic jerk. This is an involuntary twitch or startling motion just as you're falling asleep. A myoclonic jerk related to hiccups, these amusing, irritating and bizarre performances affect us asymmetrically[14] – we’re not sure why. According to a 2016 study[15], 60-70% of people experience them, whilst others[16] think they happen to everyone.
Some may also feel a falling sensation, or a sense of blinding light. Sometimes they are felt, but no motion is seen, and sometimes they can be seen by others or monitored with EEG (encephalogram), but not felt by the sleeper. When it happens, your heartbeat and breath quicken, and some people sweat. You’re more likely to experience it if you have an irregular sleep pattern, suffer from stress or anxiety, did something strenuous before falling asleep, or have dosed up on caffeine[17][18]. ...But these aren't causes – otherwise teetotallers would never get it, and it could be artificially induced with several large coffees. So what is it? Why does it happen? Although we're not sure, theories go that the sleep start is(i) to help you not fall out of a tree as you relax(ii) your body mistaking relaxation for falling out of a tree(iii) due to changes in blood pressure and body tension as you relax.In fact, nobody knows why they happen, or what their evolutionary purpose might be.
Learn more about Starting Again.



A less common syndrome that can be accompanied by a hypnic jerk is exploding head syndrome (EHS). This is a kind of recurring auditory hallucination characterised by suddenly hearing loud but non-existent short duration noises, often when falling asleep. There is a correlation between people who suffer from exploding head syndrome and people who've had sleep paralysis just once. Mostly, it happens in that stage between sleep and wakefulness. There is currently no treatment, but understanding the condition can reduce the frequency of episodes.
Theories suggest it occurs when different parts of the brain shut down at different rates and auditory neurons are activated unexpectedly; it could also represent a minor localised seizure, a stress/anxiety symptom, shift in middle-ear components, or symptom of auditory trauma.


Whilst restless legs syndrome, a discomfit experienced in the legs and knees, occurs when awake and asleep, periodic limb movement disorder, previously known as nocturnal myoclonus, occurs only during sleep. During periodic limb movements disorder, sufferers display involuntary limb movements 20–40 seconds apart for the first half of the night, before entering REM sleep where their muscles become paralysed. Movements can vary from small ankle twitches to the wild flailing of all four limbs. Symptoms also include excessive sleepiness during waking hours.
Its causes are unknown, but periodic limb movement disorder often coincides with narcolepsy and Parkinson’s, and is treated with anti-Parkinson’s medication. It is exacerbated by factors that normally affect sleep disorders, such as shift work, caffeine, stress, sleep apnea, and use of hypnotic medication.


Interestingly, some sleep disorders are more common among one sex than the other (e.g. sleep apnea in men, restless leg syndrome in women). Women are underrepresented in medical research, and so there is less data on sleep disorders that mainly or only affect women – including pregnancy- and menopause-related sleep disturbances.


 2
2
Like a(n unborn) babe
Another area of research is the relatively un-navigated territory the relationship between foetal health and maternal sleep. Some studies think that the mother can influence her child’s health by sleeping well when she’s expecting, but the cause-effect relationship between impaired sleep and infant health is a difficult web to untangle!


 3
3The sleep of unborn babies is a relatively mysterious topic: we normally measure sleep by recording brain activity, but we can’t do this for a human foetus – not whilst it's inside its mother. Researchers into brain activity instead perform EEG (electroencephogram) exams on premature babies and monitor eye movement to tell them about sleep cycles, although errors are common.


 3
3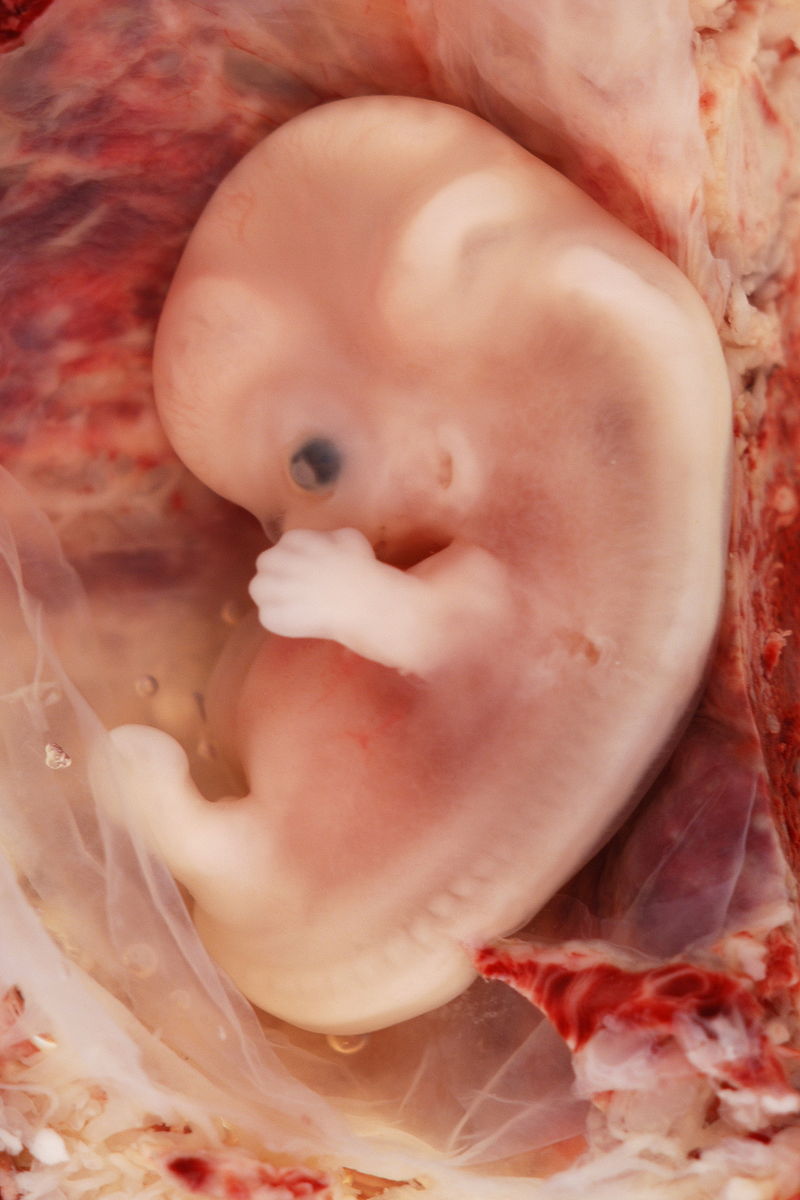


 3
3Opinion is divided when it comes to whether foetuses sleep more at night or day, and move more at night or day, although lying down can trigger movements when the baby gains space. We know they don't produce melatonin – not until 3 months or so after birth. And this makes sense: it's dark inside the womb, and there's nothing to trigger circadian rhythm. Many babies are soothed by their mother walking, and this persists after birth, with motion such as rocking sending them to sleep, whilst stillness makes them wake up. This means their night and day routine could actually be backwards!


 3
3
One thing we do know is that unborn babies do not have their limbs paralysed when they sleep to stop them from acting out their dreams. If they are indeed always sleeping or in an unconscious state as many believe, this suggests that many of their movements are involuntary or could signal something about their dreams.


 2
2Like a (newborn) babe



Many western parents are searching for that golden goose: uninterrupted infant sleep throughout the night – but is this even possible? Anthropological research throughout the world and across cultures shows that 8-12 hours of uninterrupted sleep is a peculiar western phenomenon – most humans do not sleep like this, and wake and go back to sleep several times during the night. So is our cultural expectation of sleep at fault, or is it genuinely possible to achieve this kind of sleep pattern?


Controlled crying works not because infants necessarily learn to sleep, but because they dissociate when abandoned, an adaptive response to a malevolent environment. There is an increasing amount of neuropsychology research that indicates that children who experienced controlled crying sleep training develop different behavioural-physiological profiles than those who are not exposed to this technique. This is paired with findings that indicate early infant experiences drive neural and hormonal development; immunological, hormonal and neurological functions can be depressed by distress, and despair causes harm to the structural organisation of the brain.


Co-sleeping has been demonised by SIDS networks because evidence suggests it correlates with higher levels of unexplained infant deaths. However, in western societies, approximately 50% of babies and parents co-sleep (same surface) to help baby stay down, and elsewhere as many as 100%. Anthropological research indicates that co-sleeping is beneficial in terms of feeding, nutrition and growth (for breastfed babies), attachment, and healthy neurological development. There is even research indicating that people who co-sleep as children are more independent and socially developed as young adults.
Learn more about /sids.


Case control studies on SIDS tend to be blunt instruments, categorising a whole range of different sleeping situations into a few small groups: in a cot, on a sofa, or in a bed. No one has studied the relative risks for breastfeeding-related bedsharing separately from just breastfeeding, but they have been estimated as maybe 1 or 2 per 10,000, compared to 1 per 2000 generally. This means that baby positions are not taken into account, and face down sleeping on the chest of a mother compared to a cot has not been evaluated. So far there is no evidence that sleeping face down on the chest of the mother (common co-sleeping position, also similar to baby in a sling) is any less safe than in a cot.


Infants appear to prefer sleeping on their fronts and sides to back – opposite to what is recommended by SIDS networks. We don't know why.


We think childhood sleep patterns influence adult sleep patterns (i.e. good sleepers as children tend to be good sleepers as adults and vice versa), but we don’t know for sure and we’re not sure how. It’s also not clear whether this is a nurture or nature issue – i.e. do childhood learnt patterns influence adult sleep, or is this due to innate sleep qualities, such as sleep latency periods that are genetic/inbuilt?


Beating sleep?

Many of us use caffeine to help us wake up in the morning, and it's remarkably effective. Caffeine works by blocking adenosine in the brain, making us feel more alert. But it can’t replace sleep. After a night of sleep deprivation, we experience 'rebound sleep', where we enter REM sleep earlier than we normally would, and stay in it longer.
Caffeine isn't the only drug that helps us stay awake. Patients with narcolepsy use a drug called modafinil. The same drug is also used by students, doctors and the army to help them stay awake and alert for long periods. From what we know so far, you can skip several nights sleep on modafinil without building up a sleep debt, but we don’t yet know what the long term effect might be.

Circadian rhythm
Researchers at the Sleep and Circadian Neuroscience Institute are trying to understand how the core mechanisms of sleep and 24 hour circadian rhythms are generated and regulated within the central nervous system. Understanding more about circadian rhythm could lead to therapies that help people with health conditions linked to sleep disruption, including mental illness like schizophrenia, eye disease and physical health problems.


A weird phenomenon caused by circadian rhythm is childbirth: more women go into labour in the middle of the night than during the day. The leading hypothesis is the melatonin, a hormone produced by the brain at night to help us sleep, works synergistically with the labour hormone, oxytocin, on the uterine muscle to increase the strength and intensity of contractions. The hormone oxytocin is often described as “shy”, and tends to be highest in labouring women when they are more relaxed, so this factor could also come into play.


After 150 years of cones and rods, a third light sensor has been discovered in the eye[20][21]. These non-visual photoreceptors are called photosensitive retinal ganglion cells, and act as brightness detectors, linking the internal body clock to natural light, regulating the circadian clock, making the hormone melatonin, and affecting pupil size. This means that you can still set your clocks to the external world even if you’re blind – all your rods and cones are out. And it’s important that you do – otherwise you’ll get jet-lag when your physiology (factors like alertness and hunger) get out of sync with the external world.
Researchers at the Oxford Eye Hospital are now looking at patients with genetic eye diseases to see whether their photosensitive retinal ganglion cells are okay or not – if they are, far from being told "There’s nothing more I can do for you" (or even, in some cases, going so far as to remove the eyes!), these patients will still need regular daytime light to live healthily.


Other work has found that sleep disruption always accompanies psychiatric illnesses, especially schizophrenia, bipolar, and depression. Schizophrenics, who have very disturbed sleep cycles, can significantly ease their symptoms of delusional paranoia if they are able to improve their sleep a little. The opposite has also been shown: putting a schizophrenia gene into a mouse also disrupts their sleep patterns. This works for some genes and not others (researchers aren’t yet sure why). Scientists postulate that the bits of the brain to do with sleep and mental health overlap, which means they’re using the same neurotransmitters. This means that sleep disruption may make mental illnesses worse or trigger them, and mental illness may disrupt sleep.


Sleep not only affects our mental, but also our physical health, with a wide body of research linking sleep disruption (e.g. from shift work) to factors like obesity, suppressed immunity, increased risks of cancer and coronary heart disease, and type II diabetes. Some of these may be explained by the fact that not getting enough or quality sleep can lead to hunger, which drives us to eat lots of carbs and sugar.


Sleep illnesses
Encephalitis lethargic, or the sleepy sickness (distinct from sleeping sickness), appeared as an epidemic just once, from 1916-1926. It is a multi-stage disorder characterised first by double vision, tiredness, and perhaps a fever, followed by a frozen-like state of sleeping. During this sleep, conscious victims are unable to move, and around a third die of respiratory failure. Those who wake then experience localised neurodegeneration. This is seen as a loss of motivation, willpower, and interest in life, such as the inability to appreciate beauty. Young sufferers aged 15-35 experience post-encephalitic Parkinsonism (PEP) from a few days to 30 years after the sleeping episode. Other neurologic and psychiatric changes also appear. In particular, patients became unable to control their impulses, repeatedly committing crimes like theft to little or no personal gain, and despite earlier remorse. Older sufferers escalated to self-mutilation and, upon reaching adolescence, children developed excessive sexuality and committed indiscriminate sexual assaults.
During the epidemic, doctors observed inflammation in the brainstem of patients who carried out criminal acts and showed a loss of impuse control. Doctors are still unsure how inflammation in the brainstem is linked to behavioural changes, but the discovery challenges assumed medical truths that the cortex is responsible for “higher” thinking in humans, such as a sense of self.
No virus nor bacteria has been linked with the sleepy sickness. As such, the origin of this disease, is unknown, as is the reason for its sudden disappearance. However, there is one potential clue: the outbreak followed an epidemic of the Spanish flu. Similar rare diplococcus bacteria found in sporadic modern sufferers have suggested the flu bacteria may have triggered the immune system to attack the brain – an autoimmune reaction. If true, this would mean the damage is permanent. However, the concept is controversial: a modern study on formalin-fixed, paraffin wax-embedded brain samples of encephalitis lethargica patients from 1916 to 1920 have found no signs of influenza genes[22].


 2
2
Another sleep-related disease is human African trypanosomiasis, or sleeping sickness, a vector-borne parasitic tropical disease carried by the tsetse fly that leads to flu symptoms, followed by the destruction of the central nervous system and resulting changes in personality, circadian rhythm, seizures and symptoms of stroke. Untreated, death results.
The mechanism of the disease is well known: the parasite produces tryptophol, the hormone that induces sleep. However, there are few effective treatments and no vaccine for the disease exists. Although cases have dropped from 10,000 before 2009 to 2,800 in 2015, management is due to tsetse fly confinement and eradication, and early patient screening. This is very effective as patients in more advanced stages of the disease are much harder to treat.
Recently, the parasite genome has been sequenced. The results show a complex mixture of interchangeable proteins that make the parasite hard to identify by the immune system, even once it's encountered it before. However, now identified, some of these proteins could be copied for developing targeted drugs in the future.
Tracking down the sleeping sickness is notoriously difficult. This is because whilst the tsetse fly is found in pockets all over sub-Saharan Africa, only certain species transmit the disease. And even when those potentially disease-carrying species are present, the disease itself is sometimes not. Scientists aren't sure why. Possibly fly or human resistance to the disease or poor environmental conditions are killing it off – if so, learning more could help us eliminate it.
Learn more about A sleeping sickness vaccine.


It would seem that children with ASD have different sleep patterns from other children although no-one is quite sure why.


Animal Sleep
As best as we know, all animals need to sleep; but sleep differs across the animal kingdom. Some sharks don’t seem to sleep at all, and those that do are never fully unconscious: they keep their eyes open and other senses “switched on” to pick up events happening around them. Those sharks that can pump water across their gills to get oxygen lie still and sleep deeply, but those that can't have to move to get the same flow of oxygen, and this means they literally can’t keep still: if they stop moving, they suffocate and die. When they sleep, they rest only half their brain at a time, with the other half fully alert. These sharks can voluntarily switch back and forth between brain halves. How they do this or what it feels like lies beyond our current understanding.
Learn more about How sharks sleep.


 2
2
There is good evidence that animals experience sleep problems, with genetic links to “sleep mutant” behaviours. However, animal sleep is notoriously difficult to study because the study techniques (such as use of probes) interfere with sleeping. Researchers are now using cameras to monitor sleep disruption in mice.


 2
2So that's sleep – a big topic, packed with mysteries from the how to the why, spanning the human and animal kingdoms, health, disease and behavioural science. Will we ever get to the bottom of it all?
This article was written by the Things We Don’t Know editorial team, with contributions from Jon Cheyne, Ginny Smith, Cait Percy, Rowena Fletcher-Wood, and Joshua Fleming.
This article was first published on 2019-08-21 and was last updated on 2021-07-29.
References
why don’t all references have links?
[1] Xie, L., et al., (2013) Sleep Drives Metabolite Clearance from the Adult Brain. Science 342(6156):373-377. doi: 10.1126/science.1241224.
[2] Siegel, J,M., (2009) Sleep viewed as a state of adaptive inactivity. Nature Reviews Neuroscience 10(10):747-753. doi: 10.1038/nrn2697.
[3] Berger, R,J., Phillips, N,H., (1995) Energy conservation and sleep Behavioural Brain Research 69(1-2):65-73. doi: 10.1016/0166-4328(95)00002-B.
[4] Adam, K., Oswald, I., (1984) Sleep helps healing. BMJ 289(6456):1400-1401. doi: 10.1136/bmj.289.6456.1400.
[5] Shapiro, C,M., (1981) Sleep and the athlete. British Journal of Sports Medicine 15(1):51-55. doi: 10.1136/bjsm.15.1.51.
[6] Bellesi, M., et al., (2013) Effects of Sleep and Wake on Oligodendrocytes and Their Precursors. Journal of Neuroscience 33(36):14288-14300. doi: 10.1523/JNEUROSCI.5102-12.2013.
[7] Sample, Ian. Why do we sleep? To clean our brains, say US scientists. The Guardian (18 October 2013).
[8] Fischer, S., (2005) Motor Memory Consolidation in Sleep Shapes More Effective Neuronal Representations. Journal of Neuroscience 25(49):11248-11255. doi: 10.1523/JNEUROSCI.1743-05.2005.
[9] Jewett, K.A., et al., (2015) Tumor necrosis factor enhances the sleep-like state and electrical stimulation induces a wake-like state in co-cultures of neurons and glia. European Journal of Neuroscience 42(4):2078-2090. doi: 10.1111/ejn.12968.
[10] Rasch, B. and Born, J., (2013) About Sleep's Role in Memory. Physiological Reviews. 93/ 2:681-766. doi: 10.1152/physrev.00032.2012.
[11] Eichenlaub, Jean-Baptiste, et al. (2014) Resting brain activity varies with dream recall frequency between subjects. Neuropsychopharmacology 39.7: 1594.
[12] Horikawa, Tomoyasu, and Yukiyasu Kamitani (2017). Generic decoding of seen and imagined objects using hierarchical visual features. Nature communications 8: 15037.
[13] Murray, Melissa E., et al. (2013) MRI and pathology of REM sleep behavior disorder in dementia with Lewy bodies. Neurology 81.19: 1681-1689.
[14] Fryer J. Hypnic reflex: A spinal perspective. J Sleep Disord Ther. 2014;3:5–6. doi: 10.4103/0976-3147.158797.
[15] Chiaro, Giacomo, et al. Hypnic jerks are an underestimated sleep motor phenomenon in patients with parkinsonism. A video-polysomnographic and neurophysiological study. Sleep Medicine 26 (2016): 37-44. doi: 10.1016/j.sleep.2016.07.011.
[16] Sathe, Harshal, et al. Hypnic jerks possibly induced by escitalopram. Journal of neurosciences in rural practice 6.3 (2015): 423. doi: 10.4103/0976-3147.158797.
[17] Frenette E, Guilleminault C. Nonepileptic paroxysmal sleep disorders. Handb Clin Neurol. 2013;112:857–60. doi: 10.1016/B978-0-444-52910-7.00006-4.
[18] Lozsadi D. Myoclonus: A pragmatic approach. Pract Neurol. 2012;12:215–24. doi: 10.1136/practneurol-2011-000107.
[19] Schwab et al. Nonlinear analysis and modeling of cortical activation and deactivation patterns in the immature fetal electrocorticogram. Chaos An Interdisciplinary Journal of Nonlinear Science, 2009; 19 (1): 015111. doi: 10.1063/1.3100546.
[20] Foster, Russell G. Seeing the light… in a new way. Journal of neuroendocrinology 16.2 (2004): 179-180.
[21] Van Gelder, Russell N. Non-visual photoreception: sensing light without sight. Current Biology 18.1 (2008): R38-R39.
[22] Lo, K. C., et al. (2003) Lack of detection of influenza genes in archived formalin-fixed, paraffin wax-embedded brain samples of encephalitis lethargica patients from 1916 to 1920. Virchows Archiv 442.6: 591-596.
Blog posts about sleep






Recent sleep News
Get customised news updates on your homepage by subscribing to articles













